
In India, the first “doctor” most people meet is not an MBBS in a white coat, it is a paramedic who shows up in an ambulance, a health Centre or a village lane when every second actually matters. India’s healthcare story is often told through big hospitals, specialist doctors and high end technology, but the real backbone of access is built by paramedics – the professionals who keep the system running before, beyond and alongside doctors. From accident sites and ambulances to ICUs, labs, radiology units and Health & Wellness Centers, paramedics are the crucial bridge between patients and the formal health system.
The World Health Organization has warned of a projected shortfall of around 11 million health workers globally by 2030, with low and lower middle income countries like India most affected. At the same time, India’s own human resources for health data shows that while doctors, nurses and midwives are increasing, the wider allied and paramedical workforce still needs rapid scaling to keep pace with rising demand and universal health coverage goals. In a country with a huge rural and semi urban population, paramedics are not a “nice to have” support function; they are often the only realistic way to deliver timely, affordable care at scale.
India’s paramedic gap: a silent emergency
Across reports and sector studies, one pattern is clear: India has an acute shortage of trained paramedical professionals. One widely‑quoted estimate suggests the country needs nearly 6.4 million (64 lakh) paramedics to serve the growing health sector, while current trained numbers fall significantly short. This gap shows up as over‑worked hospital teams, long diagnostic delays, and rural facilities where a single nurse or technician is expected to do everything from triage to counselling.
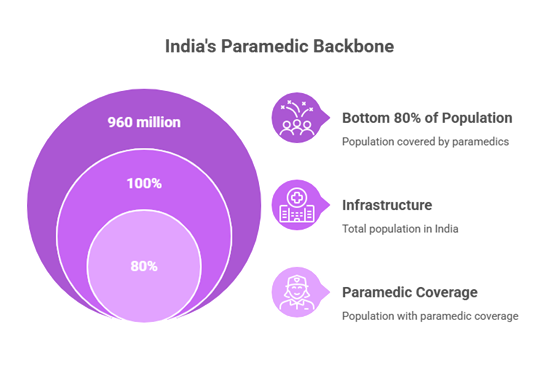
Recent health‑workforce profiling shows that while the density of doctors, nurses and midwives has improved over the last decade, the distribution remains uneven and the density of “other key primary health‑care workers” – including community‑based cadres – is still critical for reaching underserved populations. To address physician shortages, India and several states have introduced mid‑level healthcare providers (MLHPs) and community health officers at Health & Wellness Centers, explicitly recognizing that task‑sharing with trained non‑physician cadres is essential. Paramedics, allied health professionals and MLHPs together form the practical backbone that converts health infrastructure into real service coverage, especially for the bottom 80% of the population.
What paramedics actually do: from first response to ongoing care
Paramedics in India handle a wide range of roles – from emergency medical technicians (EMTs) and ICU technicians to lab, radiology, OT, anesthesia and dialysis technologists, along with community based workers who support public health programmes. They are often the true first responders in emergencies, trained to assess situations, give life saving first aid, perform CPR, manage airways, give specific emergency drugs and stabilize patients during transport. Ambulance and pre‑hospital care show their impact clearly: modern ambulances work like mini ICUs with monitors, oxygen, defibrillators and drugs, but these only save lives when a skilled paramedic is at the bedside using them effectively. In the pre hospital “golden hour” for trauma, stroke or heart attacks, paramedics turn infrastructure into survival through quick decisions, smart use of limited resources and constant updates to hospital teams.
Outside emergencies, paramedics run much of the diagnostic engine of healthcare. Lab technicians generate critical test reports, radiology technologists operate imaging equipment, and OT, anesthesia, dialysis and cardiac technicians keep surgeries and chronic‑care services going. In rural and under‑served areas, paramedics also power vaccination drives, maternal and child health programmes, disease surveillance and health education campaigns, massively extending the reach of a limited doctor workforce.
How platforms like EzeeHealth unlock the real value of paramedics
This is where EzeeHealth fits naturally into the story. While paramedics create capacity on the ground, EzeeHealth lays the digital rails that connect primary, secondary and tertiary care into one smooth, co managed journey for the patient. It works as a next‑generation co‑management platform where the general physician and super specialist share a single digital case sheet, so every referral, report and follow up stays coordinated, not fragmented.
In practice, the front line paramedic or primary care team is no longer isolated. An ECG from a small hospital, a CT report from a diagnostic center, or notes from an ambulance or PHC can be shared in real time with higher‑level hospitals, making decisions faster and more accurate, reducing bounced patients, duplicate tests and hidden costs for families, and helping scarce specialists see “worked‑up” cases. For hospitals, EzeeHealth standardizes referrals, information flow, financial settlements and follow up tracking, so paramedics and nurses spend less time chasing calls and paperwork. For patients, it feels like one continuous journey instead of a confusing maze you start with a trusted local doctor or paramedic, and when you need a higher centre, EzeeHealth silently joins the dots so that the hard work paramedics do in saving minutes and lives translates into better outcomes, fairer bills and a more humane experience in moments of crisis.
Why does this matter for India’s healthcare future?
Paramedics close three big gaps at once: they expand capacity, improve access and make care more efficient. By taking over diagnostics, emergency stabilization, routine procedures and many follow up tasks, they free doctors and nurses to focus on complex decisions and high risk cases. Evidence from India and other countries shows that well trained mid level providers and paramedics can deliver safe, high quality care at lower overall cost, with better rural retention and stronger community trust than a doctor only model. For young Indians, paramedical.
education offers a practical, job‑ready route into healthcare beyond MBBS seats, with certificate, diploma, bachelor’s and master’s programmes in areas like emergency care, lab technology, radiology, anesthesia, critical care, dialysis and physiotherapy. As technology evolves – from portable defibrillators and ventilators to telemedicine‑enabled ambulances and co‑management platforms like EzeeHealth – paramedics are being trained to use advanced tools and digital systems, pushing specialist expertise right to the last mile.
If India is serious about healthcare for all, paramedics cannot remain invisible “support staff”; they must be recognized as strategic frontline professionals, with clear standards, fair pay and strong career ladders. Investing in their education, regulation, digital enablement and rural deployment will not only close workforce gaps but also make every rupee spent on hospitals, insurance and technology work harder for patients. The country’s future – faster emergency response, stronger primary care, better chronic‑disease management and real universal health coverage – will depend on how seriously India chooses to value, train and empower its paramedics today, and on how effectively platforms like EzeeHealth help them function as an integrated, data‑driven frontline for every Indian family.
If you are a doctor and would like to explore how this could work in your practice, you can fill out a short form and the team will reach out with a personalized, step‑by‑step walkthrough.